Osteoarthritis, also known as “wear and tear” arthritis, is a progressive disease of the joints.
Cause
With osteoarthritis, the articular cartilage that covers the ends of bones in the joints gradually wears away. Where there was once smooth articular cartilage that made the bones move easily against each other when the joint bent and straightened, there is now a frayed, rough surface. Joint motion along this exposed surface is painful.
Osteoarthritis usually develops after many years of use. It affects people who are middle-aged or older. Other risk factors for osteoarthritis include obesity, previous injury to the affected joint, and family history of osteoarthritis.
Anatomy
A joint is where the ends of two or more bones meet. The knee joint, for example, is formed between the bones of the lower leg (the tibia and the fibula) and the thighbone (the femur). The hip joint is where the top of the thighbone (femoral head) meets a concave portion of the pelvis (the acetabulum).
A healthy joint glides easily without pain because a smooth, elastic tissue called articular cartilage covers the ends of the bones that make up the joint.
Symptoms
Osteoarthritis can affect any joint in the body, with symptoms ranging from mild to disabling.
A joint affected by osteoarthritis may be painful and inflamed. Without cartilage, bones rub directly against each other when the joint moves. This is what causes the pain and inflammation. Pain or a dull ache usually develops gradually over time. Pain may be worse in the morning and feel better with activity. Vigorous activity may cause pain to flare up.
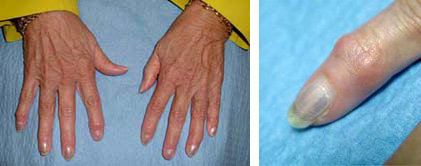
The joint may stiffen and look swollen, enlarged or “out of joint.” A bump may develop over the joint.
If bending the joint becomes difficult, motion may be limited.
Loose fragments of cartilage and other tissue can interfere with the smooth motion of joints. The joint may lock or “stick” when used. It may creak, click, snap, or make a grinding noise (crepitus). The joint may become weak and buckle.
Although osteoarthritis cannot be cured, early identification and treatment can slow progression of the disease, relieve pain and restore function.
Diagnosis
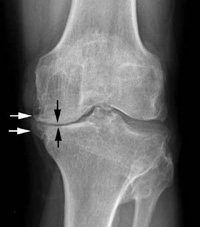
A complete medical history, physical examination, X-rays, and possibly laboratory tests will be done.
The doctor will want to know if the joint has ever been injured. He or she will want to know when the joint pain began and what the pain feels like: Is the pain continuous, or does it come and go? Does it occur in other parts of the body? It is important to know when the pain occurs: Is it worse at night? Does it occur with walking, running or at rest?
The doctor will examine the affected joint in various positions to see if there is pain or restricted motion. He or she will look for creaking or grinding noises (crepitus) that indicate bone-on-bone friction. muscle loss (atrophy), and signs that other joints are involved. The doctor will look for signs of injury to muscles, tendons, and ligaments.
X-rays can show the extent of joint deterioration, including narrowing of joint space, thinning or erosion of bone, excess fluid in the joint, and bone spurs or other abnormalities. They can help the doctor distinguish various forms of arthritis.
Sometimes laboratory tests can help rule out other diseases that cause symptoms similar to osteoarthritis.
Treatment
Nonsurgical Treatment
Early, nonsurgical treatment can slow progression of osteoarthritis, increase motion, and improve strength. Most treatment programs combine lifestyle modifications, medication, and physical therapy.
Lifestyle Modifications
The doctor may recommend rest or a change in activities to avoid provoking osteoarthritis pain. This may include modifications in work or sports activities. It may mean switching from high-impact activities (such as aerobics, running, jumping, or competitive sports) to low-impact exercises (such as stretching, walking, swimming, or cycling). A weight loss program may be recommended, if needed, particularly if osteoarthritis affects weight-bearing joints (such as the knee, hip, spine,or ankle)
Medications
Non-steroidal anti-inflammatory drugs can help reduce inflammation. Sometimes, the doctor may recommend strong anti-inflammatory agents called corticosteroids, which are injected directly into the joint. Corticosteroids provide temporary relief of pain and swelling.
Dietary supplements called glucosamine and chondroitin sulfate may help relieve pain from osteoarthritis. (Caution: The U.S. Food and Drug Administration does not test or analyze dietary supplements. Always consult your doctor before taking dietary supplements. )
Physical Therapy
A balanced fitness program, physical therapy, and/or occupational therapy may improve joint flexibility, increase range of motion, reduce pain, and strengthen muscle, bone, and cartilage tissues. Supportive or assistive devices (such as a brace,splint, elastic bandage, cane, crutches, or walker) may be needed. Ice or heat may need to be applied to the affected joint for short periods, several times a day.
Surgical Treatment
If early treatments do not stop the pain or if they lose their effectiveness, surgery may be considered. The decision to treat surgically depends upon the age and activity level of the patient, the condition of the affected joint, and the extent to which osteoarthritis has progressed.
Surgical options for osteoarthritis include arthroscopy, osteotomy, joint fusion, and joint replacement.
Arthroscopy
A surgeon uses a pencil-sized, flexible, fiberoptic instrument (arthroscope) to make two or three small incisions to remove bone spurs, cysts, damaged lining, or loose fragments in the joint.
Osteotomy
The long bones of the arm or leg are realigned to take pressure off of the joint.
Joint fusion
A surgeon eliminates the joint by fastening together the ends of bone (fusion). Pins, plates, screws, or rods may hold bones in place while they heal. This procedure eliminates the joint’s flexibility.
Joint replacement
A surgeon removes parts of the bones and creates an artificial joint with metal or plastic components (total joint replacement or arthroplasty).
